Welcome to Liverpool: stay positive. stay brilliant. stay safe.
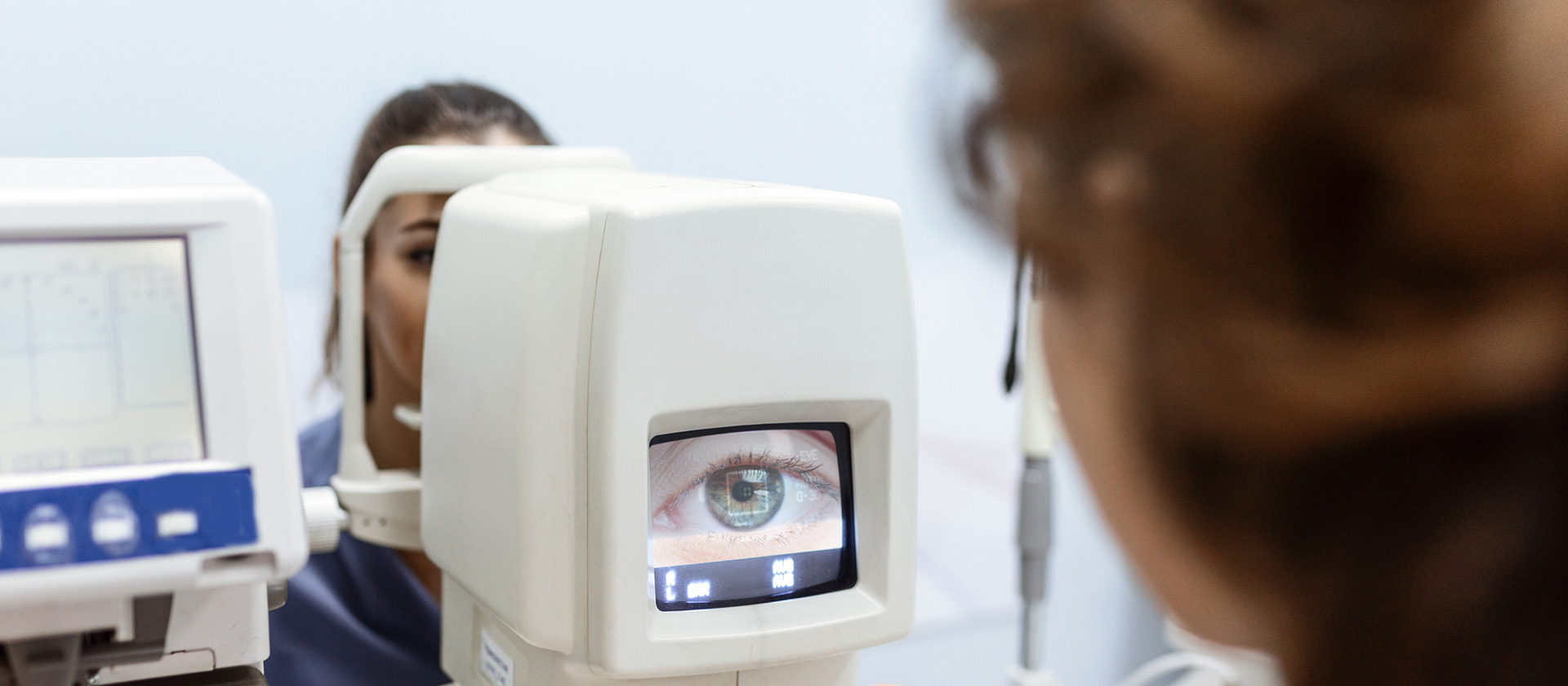
Improving the management of serious eye conditions



Glaucoma is a progressive eye disease. The damage it causes worsens over time, but early detection improves the prognosis. Researchers in the Biomechanical Engineering Group at the University of Liverpool are improving the management of this vision-threatening condition, developing more accurate techniques to avoid misdiagnosis and allow optimal treatment.
Background
Glaucoma is a leading cause of irreversible blindness, affecting 79 million people worldwide. The disease is associated with elevated intra-ocular pressure – the fluid pressure inside the eye – which causes pressure on the optic nerve head and damages the nerves that link the light-sensitive cells of the retina to the brain. The main modifiable risk factor for glaucoma is intraocular pressure, so its accurate measurement is essential for adequate treatment of the disease.
Until recently, all intra-ocular pressure measurement techniques were influenced by the stiffness of the cornea – the front window of the eye, and the resulting inaccuracies have led to both false negatives and false positives in glaucoma risk profiling. Research has shown that poor measurement has also meant that 15 per cent of glaucoma patients eventually lose their eyesight within 15 years while under treatment.
Our state-of-the-art technique for measuring internal eye pressure has been applied within a widely used commercial glaucoma diagnostic device, and have benefitted hundreds of thousands of glaucoma patients worldwide.
Professor Ahmed Elsheikh
Research
To address this challenge, researchers in the Biomechanical Engineering Group led by Professor Ahmed Elsheikh have used modelling to develop innovative methods to estimate the cornea’s biomechanical behaviour and measure intra-ocular pressure. The team has developed this technique to more accurately measure the eye’s internal pressure using a combination of experimental laboratory testing and clinical validation methods, complemented by numerical simulations of the eye (cornea) and its changes during disease and ageing.
This state-of-the-art technique for measuring internal eye pressure requires only minimal staff training because it is a non-contact device, ensuring widespread clinical implementation to save people’s sight.
Impact
The new technology that measures the eye’s internal pressure is being implemented in several clinical centres around the world. In addition to better patient outcomes, it can help to relieve the economic burden on healthcare by better and more accurate diagnosis.
While the focus at the beginning was glaucoma management, the technology has been widened to include risk profiling of keratoconus, and now ectasia, another progressive non-reversible eye condition. Early and emerging results indicate the importance of the new technique for selecting suitable patients for refractive surgery, as well as optimising use of the collagen cross-linking treatment used to prevent keratoconus progression.
Ongoing research
The University’s Biomechanical Engineering Group is also part of a European consortium of academic experts, eye clinics and companies working to develop new imaging techniques to diagnose and treat eye pathologies in a personalised manner. The IMCUSTOMEYE project, funded by the European Commission's Horizon 2020 programme, aims to implement non-invasive techniques for patients with corneal disease and glaucoma.
Despite the fact that these treatments, and the conditions they help with, interact or interfere mechanically with the cornea, there is currently no method to accurately measure corneal biomechanical properties in vivo. Such a method would be essential for customising these treatments for individual patients’ needs and ultimately improving their clinical outcomes. The IMCUSTOMEYE project is intended to address this need.
The group is currently developing two devices as part of the IMCUSTOMEYE project. The first device is an air puff based instrument that closely monitors the cornea’s deformation under an external air pressure and uses advanced mathematical and statistical techniques to determine the cornea’s biomechanical properties and estimate the eye’s internal pressure – needed for glaucoma management. The second device is intended as a screening device for keratoconus. The device monitors cornea’s response to a sound excitation and uses asymmetry in amplitudes of corneal vibration as a possible sign of the local weakness associated with the disease in its preclinical stages.
Three patent applications have been filed so far with contributions from Liverpool for different aspects of the technology, and efforts to commercialise the devices to companies within the project consortium and outside are ongoing.