CNAO - Centro Nazionale di Adroterapia Oncologica
Light ion therapy software for data exchange
Trainee: Carlos Afonso
Supervisor: Luigi Casalegno
This project was focused on creating a common software bus that enables present and future packages of the configuration and support environment of the control system to easily interconnect in a complex and widely distributed hadron therapy facility. An integral part of the project was the specification of protocols to be used in the facility’s control system configuration and support environment. These protocols should allow for data exchange, assurance of security and privacy, and discovery of devices.
In order to support the development of new applications of the configuration and support environment, a product line architecture has been designed. The architecture specifies the scope of applications, general layout, and variation points. Additionally, a wizard generator has been developed to create customized base
applications in accordance to the product-line architecture.
One of the major concerns in the medical environment is the assurance that programs and components are functioning as per specification. The Fellow has also approached the research topic of certification of the medical software, aiming at improving the certification of applications created for this project.
Novel control systems for a medical accelerator facility demand the increase of the monitoring via specification of tools that help with visualization and construction of workflows. To overcome this challenge, the next part of the Fellow’s project includes the design and development of a graphical environment that enables the description of workflows composed of several medical accelerator activities. The graphical environment is to be backed by an XML based language, allowing for the description of the workflow states and events for each connected device.
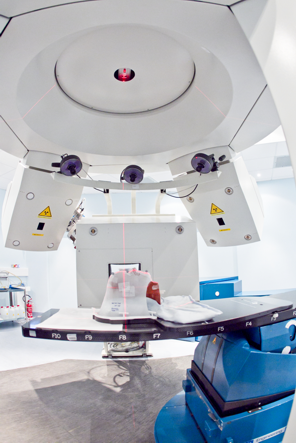
Tumour tracking in particle therapy
Trainee: Charalampos Kalantzopoulos
Supervisor: Guido Baroni
Hadron therapy is an effective method to deal with radio-resistant tumors, which cannot be treated with photon radiotherapy. The method has higher precision and better efficacy in eradicating the tumor cells than photon radiotherapy. The irradiation technique is called active scanning (or pencil) beam, due to the advantage that it can be calibrated to hit the tumor region with specific energy and penetration depth.
Despite the advantages of the procedure, a main problem arises from the interplay of the dynamic motion of the beam and the tumor motion, which may cause problems in delivering the predefined radiation dosage on the tumor cells and may potentially be harmful to the healthy tissue surrounding the area.
CT represents the clinical standard for treatment planning in both conventional and particle-based radiation therapy, with time-resolved (4D) CT being the current approach for moving organs. However, there is a growing development in the use of Magnetic Resonance Imaging (MRI) to support the clinical procedure. This is due to the advantages provided by MRI with respect to CT, such as: (i) better soft tissue contrast, which allows to improve organs delineation, (ii) absence of ionizing radiation, which allows repeated image acquisition without delivering additional dose to the patient and (iii) MR acquisition in dynamic modality, which allows to acquire internal anatomo-pathological motion over different respiratory cycles.
Within this project, the Fellow applied motion modelling strategies to MRI data for organ motion quantification in abdominal regions of patients treated with particle therapy.
Specifically, acquired sagittal/coronal 2D cine MRI data have been exploited to quantify intra- and inter-fractional variations of patients’ respiratory motion. The project explored deformable registration methods such as Optical Flow Algorithm to track the movement of the region of interest (ROI).
This allowed for the planning of treatment margins based on the motion quantified by cine MRI data, which will be compared with conventional margins defined on the 4DCT dataset. Both, geometrical and dosimetrical comparisons have been performed. The approach will be validated relying on phantom simulations or by exploiting clinical data provided by experts. Additional motion modelling techniques have been evaluated for the possibility of updating the planning CT with the motion provided by MRI data.
Image courtesy of CNAO